Hyperammonemia in the Emergency Department
Urea Cycle Disorders Consortium Treatment Guidelines
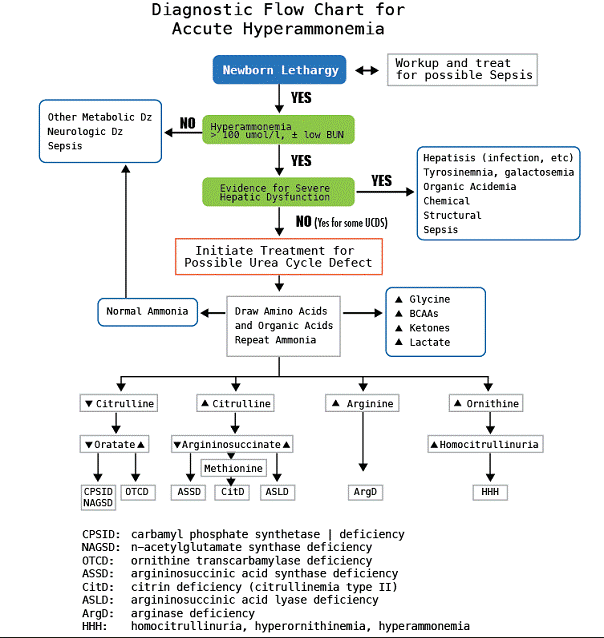
Hyperammonemia identification of Hyperammonemia in Urea Cycle Disorder and other inborn errors of metabolism
Causes of Decreased Ammonia Elimination
- Inborn error of metabolism
- Urea cycle disorders
- Lysinuric protein intolerance
- Organic aciduriasFatty acid oxidation defects
Liver failure (ASA and OTC can present with elevated liver enzymes)
Acetaminophen, steroid, or valproic acid ingestion
Symptoms
- Unexplained
- Vomiting
- Headache
- Lethargy
- Confusion
- Ataxia
- Slurred speech
- Agitation
- Unusual irritability
- Unusual behavior
- Unexplained psychosis
- Delusions or hallucinations
- Postpartum psychosis (adults)
- Stroke-like symptoms
- Hypothermia
- Respiratory alkalosis
- Irritability progressing to lethargy
- Somnolence
- Decerebrate posturing
- Coma
Presenting Symptoms in 260 UCD Patients at First Presentation of Hyperammonemia (Longitudinal Study of Urea Cycle Disorders, Urea Cycle Disorders Consortium)
- Neurologic symptoms (100%)
- Decreased level of consciousness (63%)
- Abnormal motor function or tone (30%)
- Seizures (10%)
- Vomiting (19%)
- Infection (30%)
- Subjective: Decreased appetite, fussy
- Physiologic: Respiratory alkalosis followed by apnea
History
- Protein aversion
- Loss of appetite
- Sleep disorders
- Psychiatric or behavioral disorders
- Trichorrhexis nodosa (due to dysregulated arginine)
Triggers
- Sudden onset of symptoms following high protein diet or supplements
- Catabolic state
Triggers - Causes of Increased Ammonia Production (*commonly seen in UCD)
- Virus or Infection
- Urease producing bacteria (Proteus, Klebsiella)
- Herpes
- Protein load and increased catabolism
- High protein diet or supplements
- Severe exercise
- Seizures
- Trauma or burns, massive hemolysis (large bone fracture or trauma)
- Steroid administration
- Chemotherapy
- Starvation, excessive dieting
- Gastric bypass surgery
- GI hemorrhage
- Increased renal ammonia production
- Increased splanchnic ammonia production
- Increased peripheral catabolism due to deficiency of essential amino acids
- TPN (*adults)
- Surgery
- Cancer (multiple myeloma)
Drug or supplement ingestion
- Corticosteroids (most commonly prednisone)
- Valproic acid
- Haloperidol
- Glycine
- Glutamine
- Salycilates
- Carbamazepine
- Sulfadiazine
- Pyrimethamine
- MDMA ecstasy
- Systemic antifungals
- Acetaminophen
Medical History (may include any)
- Behavioral disorder (ADD, ADHD, other), psychiatric disorder (bipolar, depression, schizophrenia)
- Poor feeding or protein avoidance
- Cyclic vomiting
- Autism
- Seizure
- Headache
- Recent drug changes (antibiotics, valproate, corticosteroids)
- Recent vaccination (triggers catabolism; effects may also be linked to preexisting mitochondrial defects in children with IEM)
- Recent surgeries (anesthesia in peds and adults, TURP in adults)
- TPN
- GI bleeding
- Urinary tract infection
Social History
- Previous death in family
- Infant (SIDS, sudden coma, unexplained encephalopathy, etc.)
- Childhood (chicken pox vaccine, DPT, unexplained encephalopathy or coma)
- Adult (sudden encephalopathy, stroke-like symptoms, psychiatric)
- Recent travel (hepatitis A, vaccination, viral infection)
- Illicit drug use
- Learning disability or developmental delay
- Unexplained lethargy or sleep disturbances
- Unusual behavior (agitation, irritability, personality change)
- Maternal history of migraine headache
Diagnostic Evaluation
- Serum Ammonia level (vacutainer on ice, run STAT)
- CBC w/differential
- CMP
- Blood cultures
- Urine and plasma amino acids
- Blood gas
Contraindications
- Lactose is not recommended for the treatment of hyperammonemia in inborn errors of metabolism.
- Corticosteroids
- Valproic acid
- Haloperidol
Disposition
Contact medical genetics/metabolic genetics immediately
- Transfer to ICU
- IV support with D10
Additional considerations (urea cycle disorders)
In addition to plasma ammonia, laboratory data useful in the diagnosis of UCDs include pH, CO2, the anion gap, blood lactate, plasma acylcarnitine profile, plasma and urine amino acids, and urine organic acid analyses including the specific determination of orotic acid. Patients with true urea cycle defects will typically have normal glucose and electrolyte levels. The pH and CO2 can vary with the degree of cerebral edema and hyper- or hypo-ventilation. In neonates it should be remembered that the basal ammonia level is elevated over that of adults, which typically is less than 35 μmol/L (less than 110 μmol/L in neonates). An elevated plasma ammonia level of 150 μmol/L (>260 μg/dl) or higher in neonates and >100 μmol/l (175 μg/dl) in older children and adults, associated with a normal anion gap and a normal blood glucose level, is a strong indication for the presence of a urea cycle defect. Quantitative plasma amino acid analysis can be used to evaluate these patients and arrive at a tentative diagnosis. Summer ML, Le Mons CL, ed. Physician’s Guide to Urea Cycle Disorders (download pdf). Online at nordphysicianguides.org/urea-cycle-disorders